First and foremost, an ENT specialist should evaluate the upper airway to determine if there is any obstruction. If the doctor suspects you are at risk for sleep apnea, you may be referred to a diagnostic sleep center for an overnight in lab sleep study, or you may receive a simple home sleep study, which utilizes mobile medical equipment to monitor your sleep. The lab then interprets the results of either study, and creates a report. Once your doctor receives the results, they will make the necessary recommendations for the best treatment options.
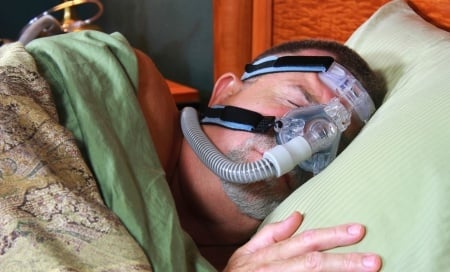
For those with mild to moderate sleep apnea, it may be as simple as clearing up the sinuses, however many people with moderate to severe sleep apnea are prescribed CPAP (continuous positive airway pressure) therapy or a dental appliance (oral appliance therapy) to push the jaw forward during sleep, which will also pull the tongue forward to prevent it from falling back into the throat. The gold standard, however, is CPAP therapy. With CPAP, the patient wears a mask at night that connects to a piece of medical equipment. The device maintains positive air pressure in the airway so it cannot collapse, making for smooth, uninterrupted breathing and restorative sleep.
Some patients may benefit from a surgery to address a particular site of obstruction
While CPAP can take time to tolerate, the equipment is much less noisy and cumbersome than it once was, and patients have a range of masks to choose from, making it even more comfortable. If you are having adjustment problems, you are not alone. In fact, most sleep apnea patients have problems tolerating the ventilation treatment and are non-compliant to CPAP therapy overall.
Your doctor may recommend an additional in-lab study called a PAP Nap, in which a patient works one-on-one with a Respiratory Therapist to improve their compliance with CPAP. A PAP Nap is a short (4-5 hour) daytime procedure designed to improve patient CPAP tolerance through education and monitored CPAP use. The referring doctor then receives a detailed report including patient’s reaction and acceptance of education and relaxation techniques, the name and size of the mask that produced the best results and a suggested setting for air pressure and other customized settings that aid in improved tolerance. This therapy effectively educates patients on the CPAP mechanisms and the benefits of CPAP therapy, helping patients cope with anxiety related to CPAP and to relax.
A common complaint patients may have when they first use CPAP is a drowning sensation. This is not a pleasant description, but that is how a lot of patients describe the feeling of sleeping with a CPAP mask. It often sets off claustrophobic and anxious responses. Sometimes, the symptoms dissipate over a period of several weeks, other times they do not.
If you find yourself experiencing a lot more of these “other times,” and you’re ready to consider an alternative to your CPAP mask, make sure to follow up with a qualified specialist to be treated for your intolerance properly.
Do not stop your treatment cold turkey and try to manage your symptoms without professional help. This never leads to a good outcome, and we want to assure that all patients being treated for sleep apnea have the best outcomes possible.
Insurance providers have very strict coverage qualifications for the treatment devices used in sleep apnea cases. You may be wondering why you have to suffer through 3 to 6 months of non-adjustment before an alternative can be discussed, but qualified practices can help with providing alternatives that are covered by insurance.
Dental appliances for example, have only been approved as an acceptable and effective treatment alternative in the last decade. That’s how long it has taken cumulative research to make a case for sleep apnea treatment to be covered by insurance.
How did the researchers do it? They collected comprehensive details on the health risks and compliance rates associated with sleep apnea.
Results: 38,000 patients die each year from health problems related to sleep apnea, yet, 85% of patients remain undiagnosed and untreated.
For now, patients can get most, if not all of their sleep study expenses paid for.
Choose between a couple of CPAP alternatives:
- Nasal ventilation device (less intrusive)
- Jaw repositioning appliance (mouth snoring only)
- Tongue retention device
Consultations are available to re-evaluate your case. eos sleep has locations in New York City and we accept most insurance plans.
